
Many lessons were learnt from the COVID-19 pandemic, but one particular point still stands out: while current vaccines have saved millions of lives, they have not completely stopped the spread of the responsible virus. One reason is that viruses evolve over time, enabling them to get around immune defences built by each infection/vaccination. But a current challenge is that these vaccines mainly trigger systemic immunity, the body-wide defence system that runs through the blood and lymphatic systems.
Systemic immune responses are excellent at preventing severe disease but may not always be good at blocking infection by pathogens at some of our bodies’ entry points. Relying on protection offered by systemic vaccines won’t be enough to prevent the next pandemic by a respiratory virus. This is where mucosal immunity comes in.
Respiratory viruses have a high chance of being the cause of the next pandemic. Credit: Yuichiro Chino/Moment via Getty Images
Body entry points such as our nose, lungs, and gut are lined with protective mucosal tissues that house the body’s frontline defence, known as our mucosal immune system. These tissues are the gateways for pathogens, such as SARS-CoV-2 the virus that causes the disease COVID-19. But the mucosal immune system is also our frontline defence.
Mucosal tissues can produce special antibodies that sit in the mucus lining the airways and neutralise viruses before they infect cells. By blocking infection at this early stage, mucosal vaccines can reduce how much virus replicates in the respiratory tract. That matters for diseases like COVID-19 which spread when infected people release virus particles through breathing, talking or coughing. If the virus cannot replicate in the nose or throat, infected people would shed far fewer viral particles, making it much harder for the virus to pass from one person to another. This is a major advance in pandemic preparedness.

Coughing is common method of transmission for respiratory viruses. Credit: Liubomyr Vorona/iStock/Getty Images Plus via Getty Images
The MUSICC project is leading efforts to understand and harness this powerful form of protection. By shifting the focus from blood-based immune responses to mucosal immunity, MUSICC aims to better understand this type of immune response and build mucosal vaccines. Facilitated through a network of experts dedicated to developing new tools, knowledge and data, this could redefine how we fight future pandemics.
The rapid development of COVID-19 vaccines during the pandemic was an extraordinary scientific achievement, saving millions of lives and reducing hospitalisations worldwide. While these vaccines were very successful in preventing severe disease, they did not completely block transmission. As a result, the virus continued to spread, sustaining risk for humans, in particular vulnerable populations, and facilitating the emergence of new variants.
Most current COVID-19 vaccines are injected into the muscle (intramuscular), where they primarily and reliably trigger a systemic immune response. This provides a whole-body immune response but does not reliably activate long-lasting immune responses in the mucosal tissues. This limitation of systemic vaccines has become increasingly clear with the rise of COVID-19 breakthrough infections and reinfections, due to lack of sterilising immunity.
Intramuscular vaccinations reliably induce systemic immune responses. Credit: Thomas Angus/Imperial College London
Systemic vaccines effectively reduce severe illness and lower the likelihood of transmission to others. But they often do not fully prevent infection leading viral transmission to continue. Without strong mucosal immunity, viruses such as SARS-CoV-2 continue to circulate, posing ongoing risk to people and creating opportunities for new variants to appear.
Recent studies have shown that while some current systemic COVID-19 vaccines may induce a mucosal immune response, it is not long-lasting. In a research paper published in Nature Communications by Mitsi and colleagues, including MUSICC’s own Daniella Ferreira, researchers commented how there are conflicting results as to whether systemic vaccines induce mucosal immunity.
When a mucosal immune response was generated by a systemic vaccine, few immune cells remained in mucosal tissues beyond seven months, even with multiple vaccines doses. By contrast, people who had both been infected and received vaccination, known as hybrid immunity, showed stronger mucosal responses. As a result, the team proposed their results supported the argument for vaccines targeting the airways.
Another study published in eBioMedicine by Liew and colleagues, including MUSICC researcher Ryan Thwaites, discussed similar results. They found that nasal IgA, a key antibody for mucosal defence, declines sharply around nine months after infection and is barely boosted by intramuscular, systemic vaccination.
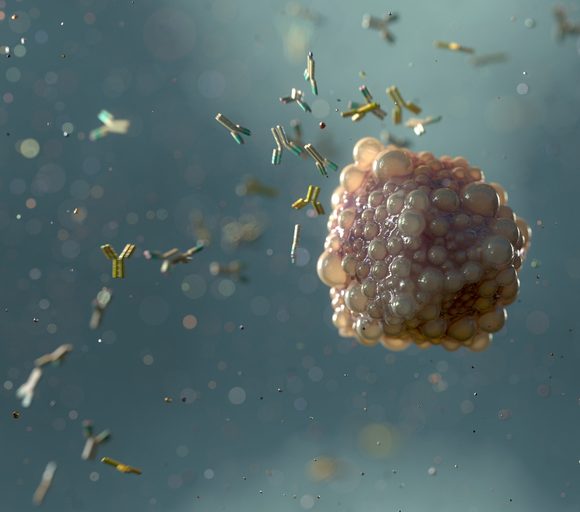
Y-shaped antibodies are a key part of mucosal immunity. Credit: Steven McDowell/Science Photo Library via Getty Images
This helps explain why systemic vaccines have limited impact on transmission: they do not sustain the immune response in mucosal tissues that blocks infection at the body’s entry points. This research team also expressed that their findings highlighted the need for vaccines that enhance nasal immunity.
Despite their success in preventing severe disease, today’s systemic vaccines leave a critical gap. This gap explains why some transmission may still persist, even in highly vaccinated populations.
Mucosal vaccines are administered directly to mucosal surfaces, for example via inhalers or nasal sprays and other methods. These methods offer a needle-free alternative to vaccines, while delivering the vaccine contents directly to where they need to be. Needle-free applications can offer a preferable alternative to individuals uncomfortable with needles, including children.

Nasal sprays are one application method for mucosal vaccines. Credit: Malikov Aleksandr/iStock/Getty Images Plus via Getty Images
Once a mucosal vaccine is applied to mucosal tissues this generates an immune response within the tissue, such as the key upper airway’s antibody IgA. Instigating immune responses in mucosal tissues empowers the body to fight pathogens at its borders before they can infect and cause disease. This, in theory, could then provide sterilising immunity, as noted by MUSICC Scientific Advisory Board member Florian Kramer in their paper published in Nature.
Interrupting this process of infection, transmission and disease prevents infected people suffering from symptoms and reduces the number of individuals that pathogens may use to make copies of themselves. This can then lead to reduced shedding, and as a result, reduced transmission of the pathogen to others. In a fast-spreading pandemic situation where we need to quickly reduce the number of infections and the speed at which a virus is infecting people, this is an incredibly powerful tool.
Limiting a pathogen’s ability to spread and make copies of itself also reduces the chances of mutations developing, which may then reduce opportunities for variants arising. Reduced variants mean less targets that vaccines and treatments need to be developed for.
As discussed in a recent report by The Wellcome Trust and The Novo Nordisk Foundation, inducing mucosal immunity holds a lot of powerful potential but there are still challenges for researchers to navigate:
Closing the gaps in mucosal immunity research requires more than incremental progress. It demands innovation across immunology, virology and vaccine technology. The MUSICC project is working to directly tackle some of the challenges currently facing mucosal immunity research.
By gathering more human-based data through a series of highly controlled human challenge studies and seeking better understanding of mucosal immunity’s correlates of protection, MUSICC is looking to lay the groundwork for this innovation.
Human challenge studies allow MUSICC to gather crucial data on coronaviruses. Credit: Thomas Angus/Imperial College London
MUSICC is an international consortium dedicated to understanding how mucosal immunity works and how we can harness it to prevent infection at the point of entry to the body. Part of the project’s mission is to understand immunology and vaccination strategies that go beyond systemic protection and help deliver long-lasting mucosal immunity.
It is very likely that the next pandemic will be caused by a virus that spreads through the air. Viruses like influenza and coronaviruses transmit easily by respiratory routes, such as breathing, coughing, sneezing or talking. Because they can then spread so quickly around the world, we need vaccines that can interrupt infection and transmission.
Mucosal immunity must be a priority; systemic immunity alone cannot stop infection at its source. To truly prevent transmission and reduce the risk of future variants, we need vaccines that work where viruses enter the body, the mucosal tissues. There may also be a case to be made for a combination of mucosal and systemic vaccines, to provide an enhanced level of protection.
Investing in mucosal vaccine research is not just a scientific imperative, but an economic and public health priority. Preventing transmission lowers healthcare costs and strengthens global health security.
Current vaccines protect against severe disease but are limited in preventing infection and reducing transmission. Mucosal immunity could be the missing piece and projects like MUSICC are working to close that gap. Investing now could help us develop vaccines that protect at the point of entry, making future pandemics easier to manage and potentially even preventable.
7th April 2026